If you’ve ever wondered how to rewire your brain from addiction, science now confirms it’s not only possible—it’s measurable and real. For decades, addiction was misunderstood as a moral failure or lack of willpower. But today, research clearly shows that addiction is a chronic brain disease that changes how your brain functions at a chemical and structural level.
Substance use affects the brain’s reward system, decision-making centers, and stress response networks. Over time, these changes reinforce compulsive behaviors, making recovery feel incredibly difficult. But here’s the encouraging part: the brain is not fixed. It’s capable of neuroplasticity—the ability to reorganize itself, form new connections, and rebuild pathways that were damaged by prolonged substance use.
Whether you’re recovering from alcohol, opioids, stimulants, or prescription drugs, learning how to rewire your brain from addiction is a critical step toward long-term recovery. With the right tools, habits, and therapeutic support, brain function can improve, emotional balance can return, and healthy behavior patterns can be restored.
This article explores the science of addiction and outlines evidence-based strategies that promote healing, strengthen the brain’s natural resilience, and support sustainable transformation—both neurologically and behaviorally.
To truly understand how to rewire your brain from addiction, it’s important to first understand what addiction actually does to the brain. Addiction is far more than just a series of bad choices or habits—it’s a chronic condition that changes how your brain operates at every level: chemically, structurally, and functionally.
Substance use affects several key brain regions, each responsible for crucial mental and emotional functions. Over time, these changes can disrupt the brain’s ability to regulate behavior, emotion, and decision-making—which explains why quitting can feel so difficult, even when the desire to stop is strong. According to the National Institute on Drug Abuse (NIDA), long-term substance use reshapes the brain in ways that make self-control harder and reinforce compulsive drug-seeking behavior.

At the core of addiction is the brain’s reward system, primarily located in the mesolimbic dopamine pathway. This system releases dopamine—a neurotransmitter associated with pleasure and motivation—when we do something beneficial, like eating or exercising.
However, addictive substances like alcohol, opioids, cocaine, and methamphetamine release dopamine in artificially high amounts. This overwhelms the system, reinforcing drug-taking behavior and teaching the brain that the substance is essential for survival—even more so than food or relationships.
Over time, natural dopamine production slows down, and the brain becomes less responsive to natural rewards. This is why people in active addiction often lose interest in hobbies, relationships, or daily responsibilities.
The prefrontal cortex is responsible for decision-making, impulse control, and long-term planning. Chronic substance use weakens this area, making it harder to resist cravings or think through consequences.
Even if someone wants to stop using, their prefrontal cortex may no longer be strong enough to override the compulsive drive triggered by the reward system.
The amygdala governs our stress response and emotional regulation. In addiction, the amygdala becomes hypersensitive, especially during withdrawal. This leads to increased anxiety, fear, and emotional instability—making relapse more likely during stressful periods.
The combination of an overactive stress system, weakened self-control, and a hijacked reward system creates a cycle that’s extremely difficult to break without support.
In short, addiction changes the brain in ways that drive compulsive behavior, reduce the ability to cope with stress, and make it harder to make healthy decisions. But thanks to the brain’s neuroplasticity, these effects aren’t permanent—and they can be reversed through intentional recovery practices.
One of the most powerful discoveries in modern neuroscience is the concept of neuroplasticity—the brain’s innate ability to change its structure and function over time in response to experience, behavior, environment, and even damage.
Contrary to outdated beliefs, the brain is not fixed after a certain age. In fact, it remains highly adaptable throughout life, especially when supported with the right conditions and interventions. This is the foundation for understanding how recovery from addiction is possible at the neurological level.
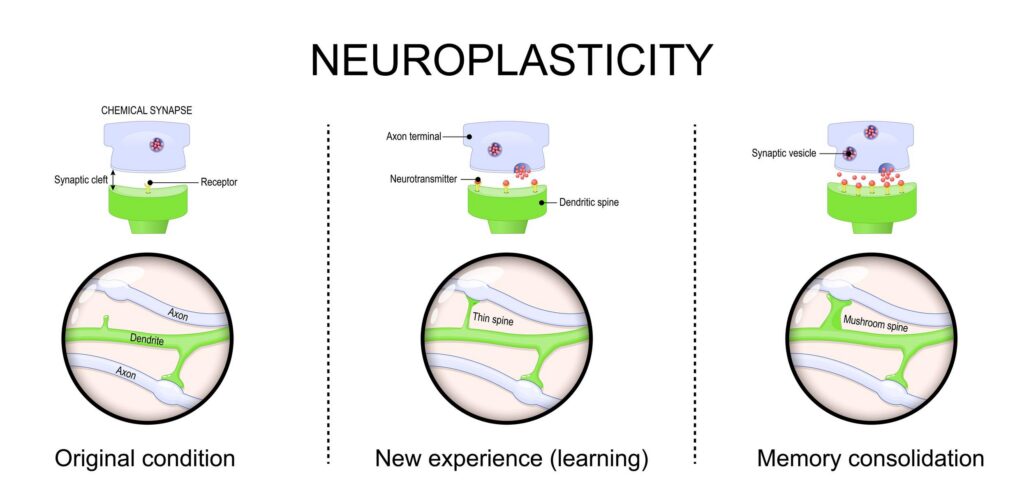
At the cellular level, neuroplasticity involves the strengthening or weakening of synaptic connections between neurons (nerve cells). These changes happen constantly as we learn, practice new skills, or shift our thinking patterns.
When you repeat a behavior or thought over time, you reinforce the neural pathways that support it. This is how habits—both good and bad—become ingrained. In addiction, these reinforced pathways link substance use to pleasure, relief, or stress coping.
But here’s the good news: just as the brain formed those pathways, it can form new ones.
With repeated exposure to healthy behaviors—like therapy, mindfulness, and exercise—the brain begins to:
This is how cognitive and behavioral recovery becomes biologically real—not just a mindset shift, but a physical transformation in the brain.
Numerous studies have confirmed neuroplasticity’s role in recovery. For example, individuals in long-term recovery from substance use show:
One study published by the National Library of Medicine observed structural brain changes—specifically, growth in gray matter—in people who had been sober from methamphetamine for just 12 months.
In short, neuroplasticity makes recovery possible. By changing your actions, thoughts, and environment, you can literally retrain your brain for healthier behavior, better decision-making, and lasting change.
Yes—scientific evidence clearly shows that it is possible to rewire your brain after addiction. Although the brain undergoes profound changes during long-term substance use, it is not permanently damaged. Through sustained abstinence, behavioral therapy, and lifestyle changes, the brain can heal—often in measurable and observable ways.
This rewiring happens because of neuroplasticity—the brain’s natural ability to reorganize its neural networks. During addiction, repeated substance use reinforces certain neural pathways, especially those linked to the brain’s reward system and stress response. But in recovery, those old pathways can weaken while new, healthier connections strengthen over time.

Brain imaging studies using fMRI and PET scans have documented remarkable changes in individuals recovering from addiction:
One widely cited study from the National Library of Medicine tracked individuals in early recovery and found that gray matter volume increased in brain regions involved in self-control and behavioral regulation.
While brain rewiring begins within weeks of abstinence, long-term healing depends on several factors:
Some people experience early gains in clarity, focus, and mood within the first 30–60 days. For others, especially those with years of heavy substance use, more significant cognitive and emotional improvements may take 12–24 months.

Rewiring the brain after addiction doesn’t happen overnight—but with the right approach, it absolutely happens. Because of neuroplasticity, the brain can change its wiring based on what we repeatedly do, think, and feel. This means that every healthy action you take in recovery is helping to reshape and strengthen your brain’s neural pathways.
Below are research-supported steps that show you how to rewire your brain from addiction in real, measurable ways.
Before any rewiring can begin, the brain must be stabilized. Detoxification is the first step in clearing the system of substances and allowing brain chemistry to start normalizing. During detox, the brain begins rebalancing dopamine, GABA, and glutamate—all critical neurotransmitters affected by addiction.
Medically supervised detox also reduces the risk of seizures, severe withdrawal symptoms, or relapse due to emotional or physical distress.
A structured treatment program provides the therapeutic environment and tools needed to begin changing how your brain responds to stress, cravings, and triggers.
Treatment should include:
Related: Overcoming Addiction: How Residential Treatment Can Help
These programs are designed to support prefrontal cortex recovery, enhance decision-making, and reduce compulsive behavior patterns.
CBT is one of the most effective therapies for addiction recovery. It works by helping you identify negative thought loops and replace them with rational, evidence-based thinking. Every time you override a harmful thought or urge, you’re literally creating new neural connections in the brain.
Long-term CBT strengthens the prefrontal cortex, improving your ability to:
This process is central to neuroplastic brain recovery.
Brains in recovery benefit from structure. A consistent routine signals safety, predictability, and reduces decision fatigue—freeing up mental energy for healing.
A healthy daily schedule might include:
Why it works: Repetition strengthens the basal ganglia, which is responsible for habit formation. Healthy routines = healthy automatic behaviors over time.
Physical activity doesn’t just improve mood—it also directly contributes to brain recovery. Exercise boosts levels of Brain-Derived Neurotrophic Factor (BDNF), a protein that promotes the growth of new neurons and strengthens existing ones.
Research published in the National Library of Medicine indicates that aerobic exercise may enhance neuroplasticity by promoting dopaminergic signaling, supporting executive function, and improving mood-related symptoms such as depression and anxiety in individuals with substance use disorders.
In animal models and human studies, exercise has also been linked to increased Brain-Derived Neurotrophic Factor (BDNF)—a key player in neuron growth and synaptic plasticity.
Recommended: 30–45 minutes of moderate-intensity aerobic activity (walking, jogging, swimming) at least 4 times a week.
Substance use depletes nutrients essential for neurotransmitter synthesis, especially those that regulate mood, focus, and motivation.
Support rewiring with:
Avoid:
Nourishing the brain helps restore dopamine balance and improve cognitive clarity.
Mindfulness reduces activity in the amygdala and increases functional connectivity between the amygdala and prefrontal cortex—helping you manage emotions more effectively.
Mindfulness techniques include:
Research published in JAMA Psychiatry found that mindfulness-based relapse prevention was significantly more effective than traditional programs in reducing relapse risk.
Just 10–15 minutes daily can lead to structural brain changes over time.
Social connection is essential for rewiring the reward system away from substances and toward human interaction, purpose, and belonging.
Options include:
Also Read: Stop Avoiding Your Emotions
Oxytocin, the “bonding hormone,” plays a role in brain repair by reducing stress and strengthening reward circuits that don’t rely on substances.
Final Thought for This Section:
Each of these steps not only supports sobriety but also contributes directly to brain rewiring through neuroplasticity. The more consistently these habits are practiced, the more deeply ingrained they become—eventually replacing old, addictive neural patterns with stable, life-affirming ones.
If you’re actively working to recover from addiction, it’s natural to wonder: how long does it take to rewire your brain from addiction? While some improvements happen quickly, full neurological recovery takes time—and varies based on several key factors.
The speed and depth of brain healing depend on:
Neuroimaging research shows that dopamine receptor activity begins to normalize within the first 90–120 days of abstinence. Improvements in prefrontal cortex function, such as decision-making and impulse control, may take longer—often 6 to 12 months or more, especially in those with severe substance use disorders.
A longitudinal neuroimaging study published in Neuropsychopharmacology found that individuals abstinent from methamphetamine for an average of 12 months showed partial recovery in dopamine transporter (DAT) availability, particularly in the striatum—a brain region critical for reward and motivation. However, the authors noted that not all functions fully normalized, and that recovery varied significantly by individual.
| Substance | Early Improvements | Significant Rewiring |
|---|---|---|
| Alcohol | 2–4 weeks | 6–12 months |
| Opioids (e.g., heroin, fentanyl) | 4–8 weeks | 12–24 months |
| Methamphetamine | 2–3 months | 18–30 months |
| Cocaine | 1–2 months | 12–18 months |
| Benzodiazepines | 6–12 weeks | 12–24 months |
These timeframes reflect average neurobiological trends—individual recovery can move faster or slower based on personal health, history, and adherence to treatment.
While some brain systems begin healing within weeks, rewiring the full spectrum of cognitive and emotional functions typically requires 6–24 months of consistent recovery work.
The takeaway? Recovery is not a straight line—but the brain responds to consistency. The more you reinforce healthy patterns, the stronger your new neural pathways become. And every step you take strengthens your ability to rewire your brain from addiction—one habit, one day, and one thought at a time.

Real-time EEG training to help regulate brainwave patterns. Improves focus, sleep, and emotional control.
Uses magnetic fields to stimulate the dorsolateral prefrontal cortex, reducing depression and enhancing executive function.
Stabilizes brain chemistry while behavioral therapies work on rewiring thought and behavior patterns.
Always used in combination with counseling and medical oversight.
Many brain functions can be restored or significantly improved. Some structural changes may persist, but neuroplasticity enables recovery over time.
There’s no shortcut, but combining therapy, exercise, nutrition, and structure is the most effective strategy.
Yes. Relapse doesn’t erase progress—it simply pauses it. Returning to treatment restarts the recovery process and reinforces neural changes.
Yes. fMRI and PET scans can show changes in brain activity, volume, and function over time, especially in research settings.
Recovery isn’t just about staying clean. It’s about changing your brain, day by day, through intentional actions, therapy, and support. Every healthy habit, every session, every connection helps forge new pathways—replacing the old ones that kept you stuck in the cycle of addiction.
Understanding how to rewire your brain from addiction is the first step. Living it—consistently, patiently, and with support—is the key to long-term healing.
Call 866-352-6898 to speak with a treatment advisor.
📋 Verify Your Insurance to begin a program that supports total brain and body recovery.
